
a 8-minute read…
The term ‘symptom modification’ is used to describe a lot of stuff therapists do to patients in an effort to reduce their pain or get them to move better immediately after, often claimed to be opening the ‘window of opportunity’ that I have discussed before. But is there any magic formula, secret recipe, procedure or standard algorithm that has to be used when trying to do this?
Now before I start I will state that I do occasionally use some symptom modification techniques for some patients, for various different things, for various different reasons. But, I also question their use a lot, as well as the common biomechanical explanations of how they allegedly work, as well as the necessity to use them in a formal standardised procedure as some advocate.
Symptom modification procedures are often associated with shoulder pain as first mentioned by Jeremy Lewis (ref) but they can cover any area such as neck, back, knee and hip pain. Symptom modification is a term that covers any intervention that a therapist does to a patient in an attempt to reduce their pain immediately, be that a joint manipulation or mobilisation, some soft tissue work, assisting or facilitating movement, taping, dry needling, even exercise and psychological interventions.
These can ALL be classed as symptom modification, as they can ALL modify a patient’s sensations and perceptions of pain stiffness, weakness and fear (Bialosky, Pickar).

Many of these symptom modification techniques are explained in purely biomechanical terms, for example, joint manipulations are said to achieve their effects via realigning joints, or creating gas bubbles. Soft-tissue techniques such as myofascial release, deep friction massages, or trigger point pressure are also said to free up tissues that are stuck or tethered together such as adhesions or scars, or they reduce muscle tone, tension, or spasm.
Some exercise-based interventions can also be seen as symptom modification by addressing so-called muscle imbalances, poor motor control, lack of stability, or improving faulty movement patterns, such as scapula dyskinesia, pelvic tilt, overactive upper traps, or underactive glutes.
How Do They Work?
Despite many claims, the simple answer is nobody really knows how any of these symptoms modification techniques work because there is always a mixture of many possible effects both biomechanical, neurophysiological, psychological, and of course contextual and placebo factors.
Of course, biomechanical factors may in part explain the modification in patients’ symptoms with these techniques… BUT… there will always be a host of other neurophysiological and psychosocial factors also contributing to how these interventions do or dont help people.
Although we can’t say with any confidence exactly how these symptom modification procedures work, we can say with more confidence how they don’t work. To put this as simply as I can lumbar spine manipulations just do NOT re-align joints that were out of place, or even alter their stiffness or flexibility much (ref, ref, ref).
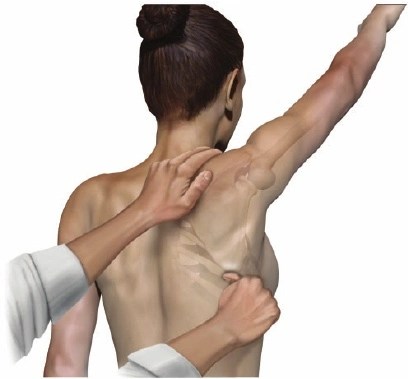
Myofascial release massage does NOT release fascia or any other connective tissue or change their mechanical properties much at all (ref, ref, ref). And although a scapula assistance test may increase its upward rotation immediately (ref), a scapula assistance test does NOT only affect a scapula, it affects the PERSON with the scapula.
We also know there is poor reliability among therapists performing many of these symptom modification techniques (VanTrijfell, Stovall), with high variability in the way they are performed and the forces under which they are applied (Snodgrass, Harms). This means that two therapists attempting to do the same technique on the same person will most likely have different results and outcomes.
Does It Matter?
However, it may not matter if we don’t know exactly how these techniques work, or if therapists do them differently because it has been shown you can apply these techniques at random and get just as good outcomes as doing the specifically (Chiradejnant, Cleland de Oliveria, Aquino, Schomacher). And just because we can’t conclusively show how these techniques work, it doesn’t mean we can’t use them.
Evidence-based physiotherapy is about working with levels of probability, and if there is evidence of a high probability of positive repeatable effects in the majority, with a low probability of risk or harm, then we can use a treatment even if we can’t fully explain how it works. However, what we do need to do is be more open and honest when it comes to explaining this uncertainty to patients about our treatments, and often this means saying…
I don’t know…
Many don’t like saying ‘I don’t know’ and I can understand this, it can be really awkward, uncomfortable and challenging to admit our ignorance to others. It can be risky as well. Patients can misconstrue it as we don’t understand what we are doing or are ill-informed. However, with some further explanation patients can understand clinician uncertainty, and often they feel better informed and so are able to make better decisions (Elwyn)
Although this uncertainty in many of our procedures and treatments can be frustrating and challenging, I think it’s also exciting and liberating as it gives us flexibility and freedom and removes the need for us to work in strict, systematic or procedural ways.
No longer do therapists only have to choose a technique based on strict biomechanical principles, or because some guru says do this before that. Therapists now have the freedom to explore many ways to modify a patient’s sensations and perceptions of pain, weakness, and stiffness based on a whole host of factors.
However, a word of warning, taking away these procedures and frameworks doesn’t give therapists the excuse to go bat shit crazy and do whatever they want using ridiculous untested interventions or other quackery. Uncertainty isn’t an excuse to fill in the unknown with whatever stupid crap you feel like.

Do We Need Procedures?
We all use systematic approaches or frameworks in many areas of our lives as it tends to make things cognitively and physically easier. This is no different in our assessments and treatments as therapists.
A methodological approach to taking a patient’s history and doing their physical examination does ensure we are thorough and efficient. For example observing an area before checking its range of movement, before checking its strength is usually a good idea. However, using a strict procedural format for your assessments and treatments is just not necessary.
People are variable, and their problems are variable, so our assessments and treatments need to be as well. If you think that when you find problem A, and you do treatment B, and you will always get outcome C, you are going to be very disappointed very quickly.
I know that procedures, frameworks and algorithms during assessment and treatments can be easier and more reassuring for clinicians, but they can also be lazier, leading to sloppiness, complacency, false beliefs and expectations, for both therapists and patients.
Should We Use Them?
As I said at the start, I use some symptom modification techniques sometimes, and I do find them helpful in reducing pain and other negative sensations and beliefs about some movements, in some patients, for a short while. They can also help some to realise that their symptoms can be changed quickly and significantly and help them feel more positive and in control of their issues.
However, I also recognise there is another not-so-helpful side of the coin with these symptom modification techniques. For some patients, these techniques can reinforce beliefs that their pain needs to be reduced before they move when in fact it’s perfectly ok and safe to move despite their pain.
They can also potentially create dependence and a loss of control and self-efficacy for some, feeling that the therapist is in control of their pain and not them. As Derek Griffin says… sometimes what a patient ‘feels’ can far outweigh anything we ‘say’.
We can also not tell which patients these symptom modification techniques will or won’t work on, and how much or for how long. And If I am being honest this is often only found out afterwards and with a bit of guesswork, clinical intuition, and a big pinch of luck.
Conclusion
So there you go, a short read on my views on symptom modification techniques and procedures. In summary, use some of these techniques on some people now and then, but throw away those procedural forms and methods and recognise there is a lot of uncertainty in how they do or don’t work.
Of course, there are many out there who disagree with this thinking or approach, usually those with their own brand of symptom modification procedures as it challenges their beliefs, teachings, and of course their weekend courses.
Some even state that this approach is reckless and even unprofessional. Some don’t like to admit that we have a lot of uncertainty in our profession and can’t fully explain the exact mechanisms of how many of our interventions work. Some like to believe they get reliable consistent results each and every time. This is not my experience and I think utter bullshit.
So do symptom modification techniques need a procedure? Well does pain have an algorithm? Do humans follow flow charts? Simply put, NO!
As always, thanks for reading
Adam
Cheers for another well written and supported blog post Adam. I feel that it’s the uncertainty and different patient responses to treatment that keeps the profession interesting, right!
Morning Adam,
Your writings are very interesting. I sometimes use symptom modification but tell patients what they really are. I think it can be useful to show patients their symptoms can be altered, but I am not sure of their true worth in the bigger picture. They occasionally have a dramatic effect, but I suspect no one really knows why. However, it is one of those terms like holistic and BPS approach that I hate as much as I like due to these terms allowing people to use quackery and drivel; an approach favoured by special interest groups interested in cognitive dissonance.
I think people like algorithms and flow charts because they offer structure and simplicity in a complex environment.
I have had shoulder pain since January. I have used myself as a guinea pig and continued my hobbies which involve high demands on the shoulder. I tried some symptom modification exercises which only helped temporarily so stopped them. At first, loading the shoulder to 3/10 did not seem to be beneficial so I changed to allow up to 8/10; gritting your teeth stuff. Things started to improve significantly then. Now almost resolved. So, in a way, the opposite of symptom modification seems to work for me. Which for me begs the question; are we faffing about too much?
Cheers for the continuing debates,
Adrian
“However, I can not tell which ones will work on which patients and if I am being honest my decision as to which technique I will apply is based on some very loose principles, some intuition, a bit of guess work and a pinch of luck.” That is so true and sometimes you get it right and sometimes your intuition fails you and you blow it…..
Top blogging. I though SSMP only related to the shoulder! I need to pull my head out of my arse.